Dupuytren’s Contracture
Patient Information
Overview
Dupuytren’s disease is a condition that causes the fascia to thicken and tightens overtime. This causes the fingers to pull inward, toward the palm, resulting in Dupuytren’s contracture. Some cases of Dupuytren’s contracture can develop to interfere with hand function, making it difficult to perform daily activities. When this occurs, patients have several options for nonsurgical and surgical procedures to help delay the progression of the disease and improve motion in the affected fingers.
Cause
The cause of Dupuytren’s disease is not completely known, but most evidence points towards genetics as having the most important role.
Risk Factors
There are a number of factors that are believed to contribute to the development or worsening of Dupuytren’s disease. These include:
-
- Gender. Men are more likely to develop the condition than women.
- Ancestry. People of northern ancestry (Viking disease) are more likely to develop the condition.
- Heredity. Dupuytren’s often runs in families.
- Alcohol use. Drinking alcohol may be associated with Dupuytren’s.
- Smoking. Smoking may increase your risk of getting Dupuytren’s disease.
- Certain medical conditions. People with diabetes and seizure disorders are more likely to have Dupuytren’s.
- Age. The incidence of the condition increases with people over 40 years of age.
Symptoms
A Dupuytren’s contracture typically progresses very slowly, over a period of years. Signs and symptoms of the condition may include:
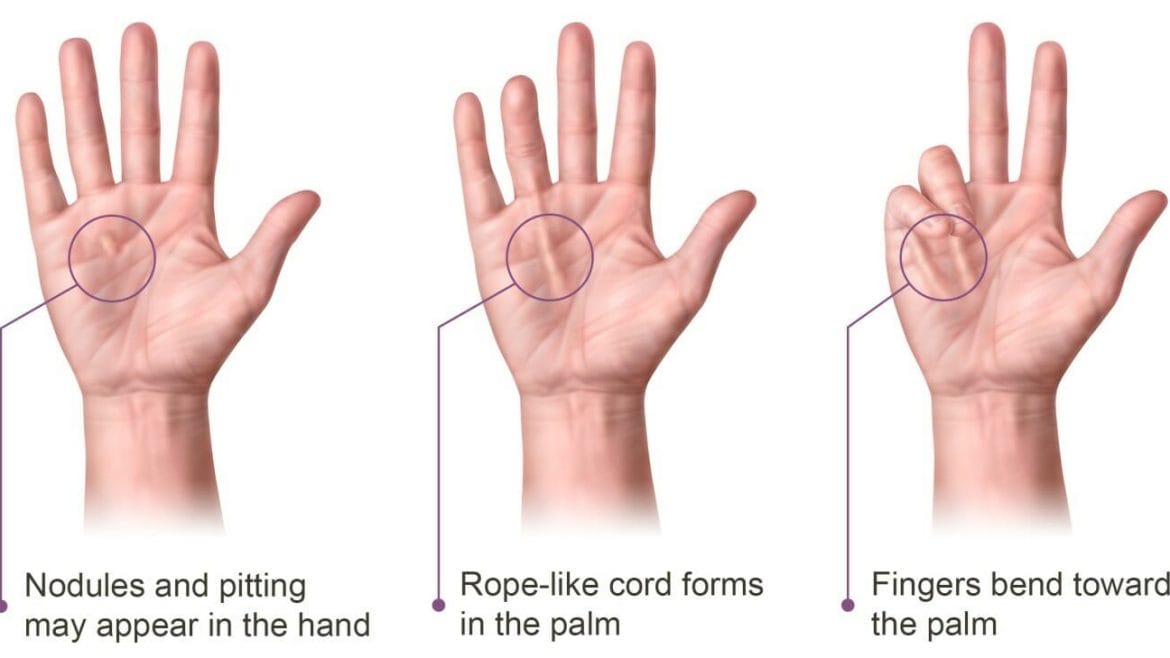
Nodules. Nodules are small lumps that may develop in the palm of the hand. These nodules typically stay in one place underneath the skin, that feel tender at first with “pitting” or deep indentation of the skin near the nodules.
Cords. The nodules may thicken and contract, contributing to the formation of dense and tough cords of tissue under the skin. These cords can restrict or tether the fingers and thumb, preventing them from straightening or spreading apart.
Contractures. As the tissue under the skin tightens one or more fingers may be pulled toward the palm, restricting motion and the ability to perform simple daily tasks. The ring and little fingers are commonly affected, but contracture can affect any finger. Most commonly, the first joint (knuckle joint) of the finger is affected, but the other joints may also be involved.
Some patients with Dupuytren’s disease may develop thickened tissue on the feet (Ledderhose disease) or penis (Peyronie’s disease). Symptoms have not been reported anywhere else on the body.
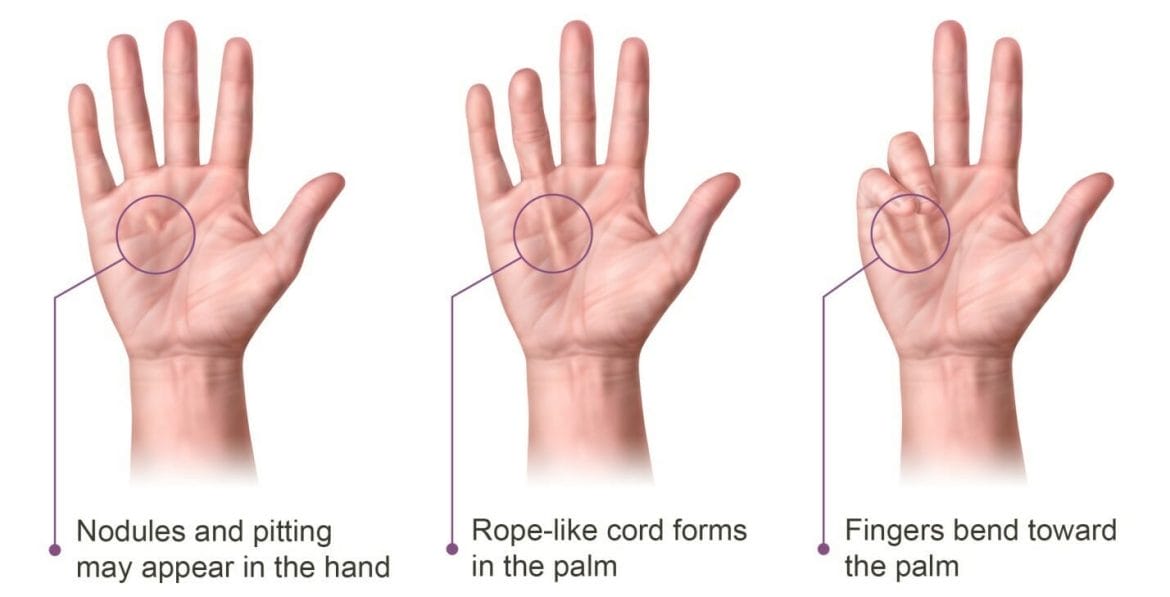
Figure 1. Illustrated common symptoms of Dupuytren’s contracture.
Doctor Examination
After checking your general health and family history (as Dupuytren’s can run in families), your doctor will carefully examine your fingers and hand.
During the exam, he or she will:
-
- Record the location of nodules and cords on your palm.
- Measure the range of motion of your fingers and thumb.
- Test the feeling in your fingers and thumb.
- In some cases, document the appearance of your hand with clinical photographs.
These measurements will be compared with later measurements taken throughout your treatment to determine whether the condition is progressing over time.
Treatment
Currently, there is no cure for Dupuytren’s. However, the condition is not dangerous, and it often progresses very slowly and might never develop beyond bothersome in most patients.
If the condition progresses, your doctor may first recommend nonsurgical treatment to help slow the disease.
Nonsurgical Treatment
Steroid injection. Corticosteroids are powerful anti-inflammatory medications that can be injected into a painful nodule. In some cases, a corticosteroid injection may slow the progression of a contracture. The effectiveness of a steroid injection varies from patient to patient.
Collagenase (Xiaflex) injection. The enzymes (purified collagenase clostridium histolyticum) was the traditional treatment for Dupuytren ‘s Contracture as it is effective in breaking down the cord, but not the surrounding tissues in the hand. This procedure to straighten out the fingers includes 3 different steps: 1. Xiaflex Injection, 2. Follow-up for finger extension procedure, and 3. Splint fabrication.
Splinting. Splinting is not known to prevent the progression of a finger contracture. In fact, forceful stretching of the contracted finger could cause an injury to the finger or hand. Splinting may be used after surgery for Dupuytren’s contracture to protect the surgical site; however, it is not known if it reduces the risk of recurrent contracture or tightening of the healing wound.
Surgical Treatment
If the contracture interferes with hand function, your doctor may recommend surgical treatment to improve motion in the affected fingers. Although surgery will not cure Dupuytrent’s disease, it helps reduce the restricting effect of the cords by either disrupting or removing them. Unfortunately, the healing tissues will form with the same potential to develop cords in the future, but the gains in hand function can still be substantial. Your doctor will discuss which procedure is best in your case.
The surgical procedures most commonly performed for Dupuytren’s contracture are:
Needle Aponeurotomy. In this procedure, your doctor will sterilize and numb an area on the affected hand. He will insert a needle into the tissue causing the pulling to make several holes in the tissue. This will allow him to straighten your fingers as the tissue expands and releases the pull on your fingers. Afterwards, he will inject your hand with a steroid medicine to reduce swelling.
Fasciotomy. In this procedure, your doctor will numb your hand with local anesthesia then make an incision in your palm to divide the thickened cord(s) of tissue. Although the cord itself is not removed, dividing it helps to decrease the contracture and increase movement of the affected finger(s). After the procedure, your wound will be left open and allowed to heal gradually. You will have to wear a splint during your recovery.
Subtotal palmar fasciectomy. In this procedure, your doctor will often make a “zig-zag” incision along the natural creases of your hand, then remove as much of the abnormal tissue and cord(s) as possible in order to straighten your finger(s). In some cases, your wound will be left open to heal gradually on its own after fasciectomy. In other cases, a skin graft will be needed to help the wound heal. In this case, your doctor will take healthy skin from another area of your body and use it to seal the wound. You may have to wear a splint during your recovery for both cases.
Subtotal palmar fasciectomy is a more extensive procedure than fasciotomy as it entails more wound care and physical therapy, a longer healing time, and greater patient effort during recovery.
Complications
As with any surgery, there are risks associated with surgery for Dupuytren’s contracture. The likelihood of complications increases with the following:
-
- The severity of the contracture
- The number of contractures addressed in a single procedure
- The presence of any other medical conditions
Your doctor will discuss each of the risks with you and will take specific measures to help avoid potential complications. Possible risks and complications of surgery for Dupuytren’s include:
-
- Recurrence
- Pain
- Scarring
- Injury to nerves and/or blood vessels
- Wound infection
- Stiffness
- Loss of sensation. Temporary loss of sensation may result from stretching nerves that have been contracted for a long time.
- Loss of viability of a finger/loss of a finger (rare)
Recovery
Severe problems are not common after surgery, but you should expect some pain, swelling, and stiffness. Although the goal of surgery is to improve digital straightening, sometimes patients can lose flexion of the involved digits due to stiffness. Elevating your hand above your heart and gently moving your fingers will help decrease swelling and should improve stiffness.
Physical therapy can help improve strength and function in your fingers and hand, reduce swelling, and aid in wound care. Often, a hand therapist will make a splint for you to wear during recovery.
Outcomes
Most patients have improved movement in their fingers after surgery. However, because the condition is not “cured” with surgery, about 20 percent of patients will experience contracture recurrence. Additional surgery may be required for some patients.
References:
OrthoInfo. (2020). Diseases & conditions: Dupuytren’s disease. Retrieved from https://orthoinfo.aaos.org/en/diseases–conditions/dupuytrens-disease/Orthopaedic & Neurosurgery Specialists. (2020). Xiaflex treatment for dupuytren’s contracture.
Retrieved from https://onsmd.com/wp-content/uploads/sites/43/2015/12/Xiaflex-Treatment_Final.pdf
Michigan Medicine University of Michigan. (2019). Needle aponeurotomy for dupuytren’s disease. Retrieved from https://www.uofmhealth.org/health-library/abp3208
Fig. 1. Clifford Craig Foundation. (2018). Dupuytren’s disease: Research update. Retrieved March 31, 202 from https://cliffordcraig.org.au/dupuytrens-disease-research-update/